According to widely cited industry estimates, the cost of one hour of downtime in critical healthcare systems can easily exceed hundreds of thousands of dollars, considering operational disruptions, clinical rework, and regulatory risks.
However, in the healthcare sector, the impact of a digital failure goes far beyond financial or reputational damage: it can directly affect real patients, delay diagnoses, interrupt treatments, or force clinical decisions to be made with incomplete information.
Healthcare systems monitoring has therefore become a critical pillar for the operation of clinics, hospitals, laboratories, and healthtech platforms. Today, medical appointment platforms, access to laboratory results, and telemedicine services are an essential part of the healthcare ecosystem. Ensuring their availability, stability, and reliability requires going beyond traditional monitoring and adopting predictive approaches, anomaly detection, and continuous validation of critical workflows.
In this article, we explore how advanced healthcare systems monitoring makes it possible to prevent incidents before they impact patients, protect operational continuity, and why, in this sector, digital reliability is non-negotiable.
In other contexts, a system outage can be resolved with apologies and compensation. In healthcare, the consequences are far more serious. A system outage can mean:
- Patients unable to schedule an urgent appointment
- Laboratory results inaccessible
- Physicians lacking critical information to make decisions
- Disruptions to telemedicine consultations
- Overloaded phone lines and in-person support channels
For this reason, healthcare systems monitoring must be designed around a fundamental principle: incidents must be prevented, not just resolved.
Modern healthcare platforms are highly complex. They are not a single application, but rather a collection of interconnected systems:
- Patient portals
- Appointment management systems
- Laboratory results platforms
- Integrations with clinical systems
- Interoperable APIs
- External and government services
Each dependency increases operational risk. A small failure in one integration can propagate and affect multiple services. This is where healthcare systems monitoring becomes essential to maintain control and visibility.
This interdependence represents an inherent operational risk in microservices architectures (or service mesh architectures, where applicable) used by modern healthtech platforms.
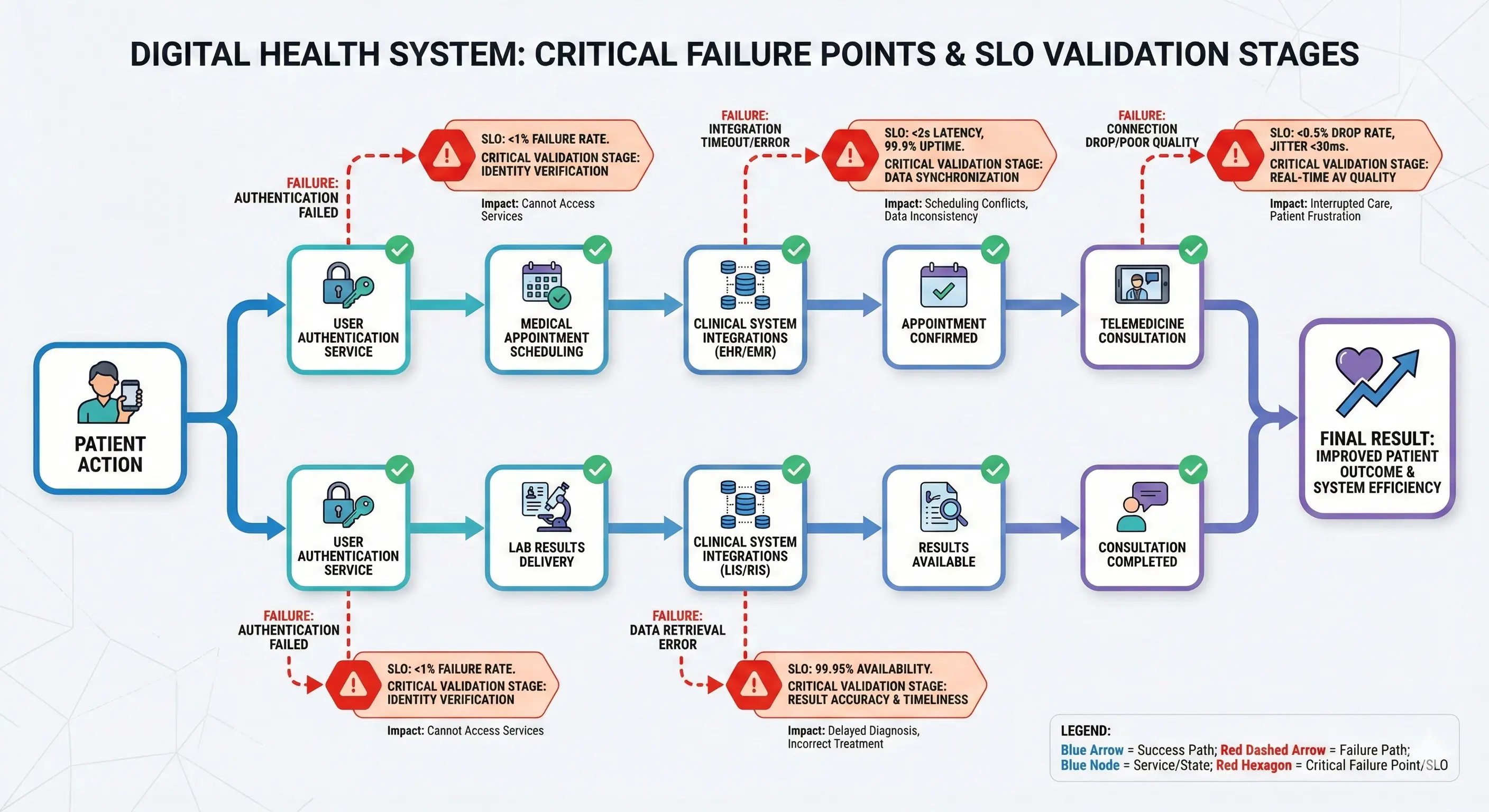
To ensure reliability, it is crucial to identify where digital healthcare systems most commonly fail.
Unavailability of the appointment system leads to delays, lost slots, and immediate patient frustration.
Delays or failures in delivering results can affect diagnoses and treatments.
Issues with identity, tokens, or validations prevent access to sensitive medical information.
An interruption during a virtual consultation directly affects patient care.
Interoperability errors can result in incomplete or inconsistent data.
Healthcare systems monitoring must focus especially on these critical points.
Most incidents on healthcare platforms do not happen abruptly. Early warning signals usually appear before an outage.
- Gradual increases in latency
- Slower responses in medical queries
- Delays in loading results
- Sporadic failures when scheduling appointments
- Access that works for some users but not for others
AI-based anomaly detection makes it possible to identify these unusual patterns before they become visible incidents for patients or medical staff. In healthcare systems monitoring, this capability makes the difference between preventive correction and an operational crisis.
What does AI detect that traditional monitoring does not?
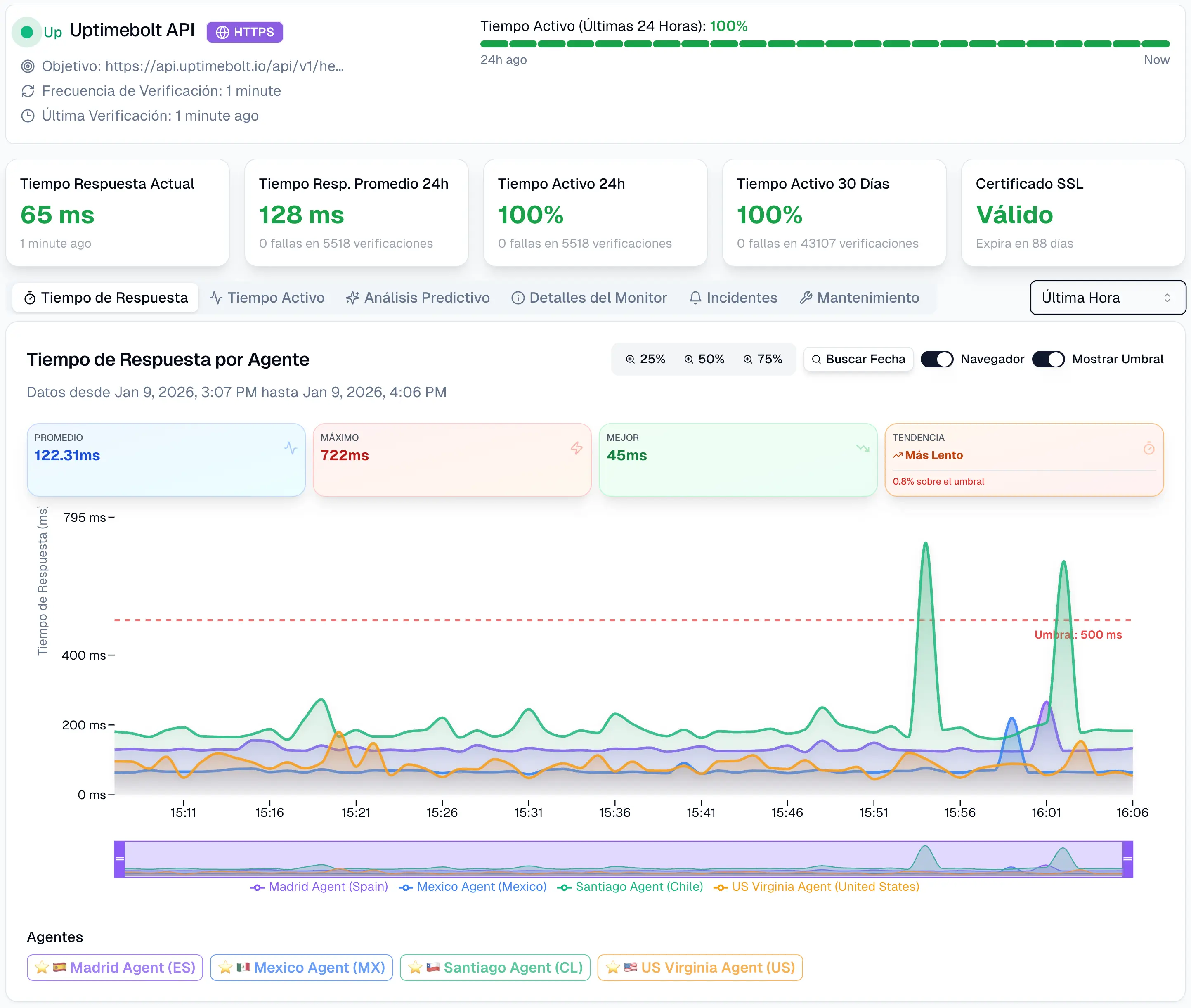
A subtle 15% increase in the error rate of the /api/results endpoint only in the Madrid region, while global latency remains normal—indicating a segmented failure.
Synthetic monitoring is especially valuable in medical platforms because it validates complete workflows from the system’s perspective.
For a complete view, teams should correlate Synthetic Monitoring (continuous system validation) with RUM (Real User Monitoring) to understand the real patient experience. UptimeBolt integrates both perspectives.
It is important to clarify that synthetic monitoring does not measure real user behavior (that is the role of RUM), but instead simulates users to validate real system behavior in a controlled way.
In healthcare, the most critical workflows typically include:
- Scheduling an appointment
- Confirming the appointment
- Accessing laboratory results
- Downloading reports
- Starting a telemedicine consultation
Synthetic monitoring makes it possible to continuously verify that these workflows function correctly, even when no users are actively using the system.
Interoperability is a key characteristic of the modern healthcare ecosystem. Standards such as HL7 and FHIR enable different systems to share clinical information, but they also introduce new risks.
Healthcare systems monitoring must include:
- Latency and availability of clinical APIs
- Validation of response content
- Detection of timeouts or silent errors
- Monitoring of external integrations
A slow or inconsistent API can generate incomplete data in clinical systems, directly affecting patient care.
In healthcare, reliability and security are deeply interconnected. An unstable system not only causes downtime, but also introduces security risks:
- Excessive retries
- Inconsistent states
- Incomplete processes
- Risks of unauthorized access
Healthcare systems monitoring helps detect anomalous behaviors that may indicate both operational failures and potential security incidents, making monitoring a key tool for regulatory compliance and sensitive data protection.
In healthcare, uptime is not just a technical metric. It is a direct indicator of trust.
A patient who cannot access their results or schedule an appointment loses confidence in the institution, even if the issue was brief. For this reason, healthcare systems monitoring must focus on real uptime—the system’s ability to fulfill its function when the patient needs it.
This concept is known as Business Uptime, the most relevant reliability metric for leadership, because it measures whether the system is fulfilling its business function (for example, scheduling an appointment), not just whether a server responds to a ping.
Many healthcare systems still rely on reactive monitoring: they become aware of problems only when patients start calling or complaining.
A modern approach combines:
- Reactive monitoring to detect visible failures
- Predictive monitoring to anticipate incidents
- Anomaly detection to identify early degradations
This hybrid approach is key to reducing incident impact and protecting service continuity.
UptimeBolt is designed to support healthcare systems monitoring in environments where reliability is critical.
The platform enables:
- Synthetic monitoring of critical medical workflows
- Monitoring of APIs and clinical integrations
- AI-powered anomaly detection
- Incident prediction before patients are affected
- Intelligent alerts with clear, actionable context
- Event correlation to accelerate diagnosis
This approach allows clinics, hospitals, and healthtech platforms to anticipate issues, reduce operational impact, and protect the patient experience.
If you want to improve the reliability of your healthcare platforms and prevent incidents before they affect patients, sign up and get a free trial.
Healthcare systems monitoring is not a luxury or a technical optimization. It is a direct responsibility to patients, professionals, and healthcare organizations.
Ensuring reliability across appointment platforms, access to clinical results, and telemedicine requires anticipation, continuous validation, and intelligent use of data. With predictive monitoring, anomaly detection, and critical workflow simulation, it is possible to identify problems before they become serious incidents that affect patient care.
Moreover, high digital reliability is a key pillar of operational continuity and regulatory compliance. In environments governed by frameworks such as HIPAA or European data protection regulations, downtime, silent degradation, or loss of traceability generate not only clinical impact but also legal and reputational risk.
In the healthcare sector, digital reliability is non-negotiable. And organizations that treat it as a strategic priority are better prepared to comply with regulations, sustain operations, and protect what matters most: people’s lives and trust.
According to widely cited industry estimates, the cost of one hour of downtime in critical healthcare systems can easily exceed hundreds of thousands of dollars, considering operational disruptions, clinical rework, and regulatory risks.
However, in the healthcare sector, the impact of a digital failure goes far beyond financial or reputational damage: it can directly affect real patients, delay diagnoses, interrupt treatments, or force clinical decisions to be made with incomplete information.
Healthcare systems monitoring has therefore become a critical pillar for the operation of clinics, hospitals, laboratories, and healthtech platforms. Today, medical appointment platforms, access to laboratory results, and telemedicine services are an essential part of the healthcare ecosystem. Ensuring their availability, stability, and reliability requires going beyond traditional monitoring and adopting predictive approaches, anomaly detection, and continuous validation of critical workflows.
In this article, we explore how advanced healthcare systems monitoring makes it possible to prevent incidents before they impact patients, protect operational continuity, and why, in this sector, digital reliability is non-negotiable.
In healthcare, a digital failure can affect real lives
In other contexts, a system outage can be resolved with apologies and compensation. In healthcare, the consequences are far more serious. A system outage can mean:
For this reason, healthcare systems monitoring must be designed around a fundamental principle: incidents must be prevented, not just resolved.
The growing complexity of digital healthcare systems
Modern healthcare platforms are highly complex. They are not a single application, but rather a collection of interconnected systems:
Each dependency increases operational risk. A small failure in one integration can propagate and affect multiple services. This is where healthcare systems monitoring becomes essential to maintain control and visibility.
This interdependence represents an inherent operational risk in microservices architectures (or service mesh architectures, where applicable) used by modern healthtech platforms.
Critical points in healthcare platforms
To ensure reliability, it is crucial to identify where digital healthcare systems most commonly fail.
Medical appointments
Unavailability of the appointment system leads to delays, lost slots, and immediate patient frustration.
Laboratory results
Delays or failures in delivering results can affect diagnoses and treatments.
Validation and authentication
Issues with identity, tokens, or validations prevent access to sensitive medical information.
Telemedicine
An interruption during a virtual consultation directly affects patient care.
Clinical integrations
Interoperability errors can result in incomplete or inconsistent data.
Healthcare systems monitoring must focus especially on these critical points.
How to detect anomalies before they affect patients
Most incidents on healthcare platforms do not happen abruptly. Early warning signals usually appear before an outage.
Performance anomalies
Intermittent errors
AI-based anomaly detection makes it possible to identify these unusual patterns before they become visible incidents for patients or medical staff. In healthcare systems monitoring, this capability makes the difference between preventive correction and an operational crisis.
What does AI detect that traditional monitoring does not?
A subtle 15% increase in the error rate of the
/api/resultsendpoint only in the Madrid region, while global latency remains normal—indicating a segmented failure.Synthetic monitoring of critical healthcare workflows
Synthetic monitoring is especially valuable in medical platforms because it validates complete workflows from the system’s perspective.
For a complete view, teams should correlate Synthetic Monitoring (continuous system validation) with RUM (Real User Monitoring) to understand the real patient experience. UptimeBolt integrates both perspectives.
It is important to clarify that synthetic monitoring does not measure real user behavior (that is the role of RUM), but instead simulates users to validate real system behavior in a controlled way.
In healthcare, the most critical workflows typically include:
Synthetic monitoring makes it possible to continuously verify that these workflows function correctly, even when no users are actively using the system.
API monitoring in interoperable healthcare systems
Interoperability is a key characteristic of the modern healthcare ecosystem. Standards such as HL7 and FHIR enable different systems to share clinical information, but they also introduce new risks.
Healthcare systems monitoring must include:
A slow or inconsistent API can generate incomplete data in clinical systems, directly affecting patient care.
Security and operational reliability: a dual responsibility
In healthcare, reliability and security are deeply interconnected. An unstable system not only causes downtime, but also introduces security risks:
Healthcare systems monitoring helps detect anomalous behaviors that may indicate both operational failures and potential security incidents, making monitoring a key tool for regulatory compliance and sensitive data protection.
Real uptime and its impact on patient trust
In healthcare, uptime is not just a technical metric. It is a direct indicator of trust.
A patient who cannot access their results or schedule an appointment loses confidence in the institution, even if the issue was brief. For this reason, healthcare systems monitoring must focus on real uptime—the system’s ability to fulfill its function when the patient needs it.
This concept is known as Business Uptime, the most relevant reliability metric for leadership, because it measures whether the system is fulfilling its business function (for example, scheduling an appointment), not just whether a server responds to a ping.
Incident prevention versus late reaction
Many healthcare systems still rely on reactive monitoring: they become aware of problems only when patients start calling or complaining.
A modern approach combines:
This hybrid approach is key to reducing incident impact and protecting service continuity.
How UptimeBolt prevents incidents in healthcare platforms
UptimeBolt is designed to support healthcare systems monitoring in environments where reliability is critical.
The platform enables:
This approach allows clinics, hospitals, and healthtech platforms to anticipate issues, reduce operational impact, and protect the patient experience.
If you want to improve the reliability of your healthcare platforms and prevent incidents before they affect patients, sign up and get a free trial.
Conclusion: in healthcare, reliability is not optional
Healthcare systems monitoring is not a luxury or a technical optimization. It is a direct responsibility to patients, professionals, and healthcare organizations.
Ensuring reliability across appointment platforms, access to clinical results, and telemedicine requires anticipation, continuous validation, and intelligent use of data. With predictive monitoring, anomaly detection, and critical workflow simulation, it is possible to identify problems before they become serious incidents that affect patient care.
Moreover, high digital reliability is a key pillar of operational continuity and regulatory compliance. In environments governed by frameworks such as HIPAA or European data protection regulations, downtime, silent degradation, or loss of traceability generate not only clinical impact but also legal and reputational risk.
In the healthcare sector, digital reliability is non-negotiable. And organizations that treat it as a strategic priority are better prepared to comply with regulations, sustain operations, and protect what matters most: people’s lives and trust.